You are viewing 1 of your 1 free articles. For unlimited access take a risk-free trial
Tender tendons: could your medication injure you?

SPB highlights research showing that fluoroquinolone antibiotics pose a potentially serious risk for athletes in training
The development of antibiotics is without doubt one of mankind’s greatest scientific achievements, saving countless millions of lives since their introduction. However, notwithstanding the current concerns about ‘superbug’ resistance, not everything is rosy in the antibiotic garden. This is because there's been steadily accumulating evidence that one particular group of antibiotics - fluoroquinolones – might be implicated in rapid-onset tendon degeneration, exposing sportsmen and women to an increased risk of tendonitis or even tendon rupture.What are fluoroquinolones?
Fluoroquinolones are effective, broad-spectrum antibiotics first developed in the 1970s, which play an important role in the treatment of serious bacterial infections such as pneumonia, typhoid, diarrhoea, kidney/urinary tract infections and many other stubborn and virulent infections. Indeed, some of the more recent iterations of fluoroquinolones are particularly effective against bacteria such as Staphylococcus Aureus and Staphylococcus Pneumoniae, which have become resistant to many other antibiotics.The fluoroquinolones (see figure 1) are a subgroup of the larger quinolone family of antibiotics. All quinolones work by preventing bacterial DNA from unwinding and duplicating. Examples of commonly used fluoroquinolone antibiotics include ciprofloxacin, levofloxacin, norfloxacin and gemifloxacin. All the fluoroquinolones share the same essential chemical structure (shown in figure 1 below). The ‘F’ denotes the fluorine atom (giving rise to the ‘fluoro’ in fluoroquinolones), while the ‘R’ denotes the chemical side group – it’s the different R groups that produce the different types of fluoroquinolone antibiotics.
Figure 1: Fluoroquinolone structure
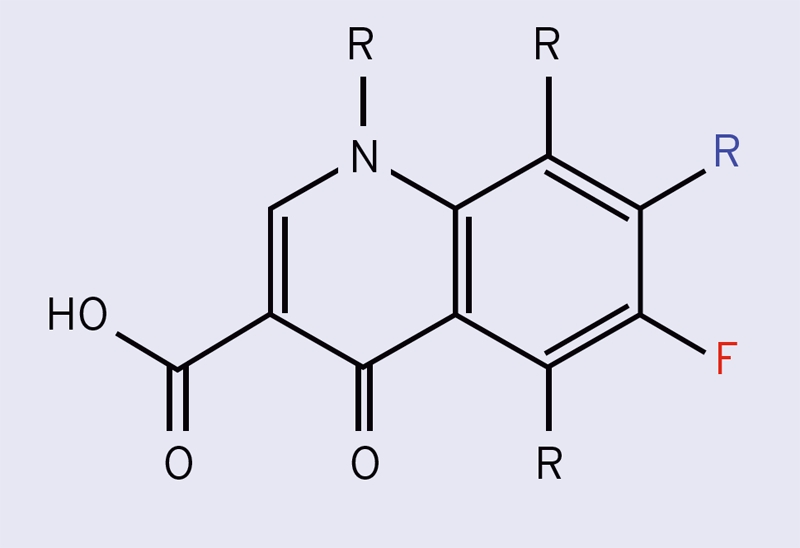
NB: ‘F’ represents the fluorine atom common to all fluoroquinolones while the blue ‘R’ group is the side chain of atoms determining the exact type of antibiotic that results.
Fluoroquinolone concerns
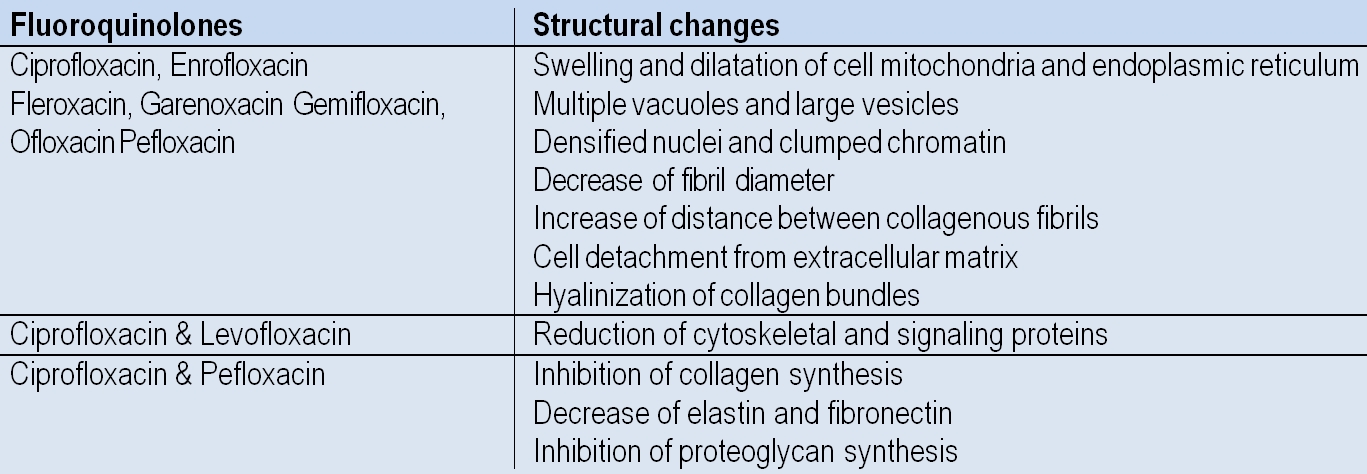
Hailed by some as ‘wonder antibiotics’, fluoroquinolone use by physicians increased dramatically towards the turn of the century. In the late 1990s however, evidence began to emerge linking fluoroquinolone antibiotic use with structural changes at the cellular level to connective tissue in the body – particularly to collagen, a major and vital component of tendon tissue.Many of the initial findings came about as a result of studies on rats (see table 1)(1-6). However, studies on human cell samples seemed to indicate that by causing a decrease in essential components of tendon tissue such as collagen type I, elastin, fibronectin and proteoglycan, fluoroquinolone-induced degenerative structural changes to tendon tissue were also possible in human tendon tissue(7).
Table 1: Structural and biochemical changes in tendon cells induced by fluoroquinolones(1-6)
Around about the same time, a growing number of tendonitis and tendon rupture cases were being observed among patients taking fluoroquinolone antibiotics. A 2003 Canadian study of 98 case studies found that pefloxacin and ciprofloxacin were most frequently implicated, but tendon injury had been reported with most fluoroquinolones(8). The median duration of fluoroquinolone treatment before the onset of tendon injury was eight days, although symptoms occurred as early as two hours(!) after the first dose and as late as six months after treatment was stopped. Up to one-half of patients experienced tendon rupture, and of these almost one third had also received long-term corticosteroid therapy before or during fluoroquinolone use.
As concern over the association between fluoroquinolone use and tendonitis/tendon rupture grew, the US FDA issued a general alert on the risks of fluoroquinolone use stating(9): “Tendinitis and tendon rupture most frequently involves the Achilles tendon, and rupture of the Achilles tendon may require surgical repair. Tendinitis and tendon rupture in the rotator cuff, the hand, the biceps, and the thumb have also been reported. Tendon rupture can occur during or after completion of fluoroquinolone use; cases occurring up to several months after completion of therapy have been reported. Fluoroquinolones should be discontinued if the patient experiences pain or inflammation in a tendon (symptoms that may precede rupture of the tendon), or tendon rupture."
For athletes undergoing strenuous training, tendon aches, pains and niggles are of course relatively common. However, fluoroquinolone-induced tendon damage tends to be quite different in the way it presents. Athletes who take or have recently (in the past six months) taken fluoroquinolone antibiotics (and their coaches) should therefore be aware of the typical clinical manifestations of this kind of tendon damage. These signs include(10):
- The weight-bearing Achilles tendon is most commonly affected, occurring in over 90% percent of cases.
- An abrupt onset and sharp pain that occur spontaneously upon walking or palpation (manually placing pressure) of the tendon.
- The occurrence of a spontaneous pain at the bony insertion 2-3 centimeters above the tendon insertion point on the bone. In the case of the Achilles, this would be at the bottom of the tendon, near the heel bone.
- Pain, swelling, or inflammation in the tendon area (often occurs for up to two weeks before rupture occurs).
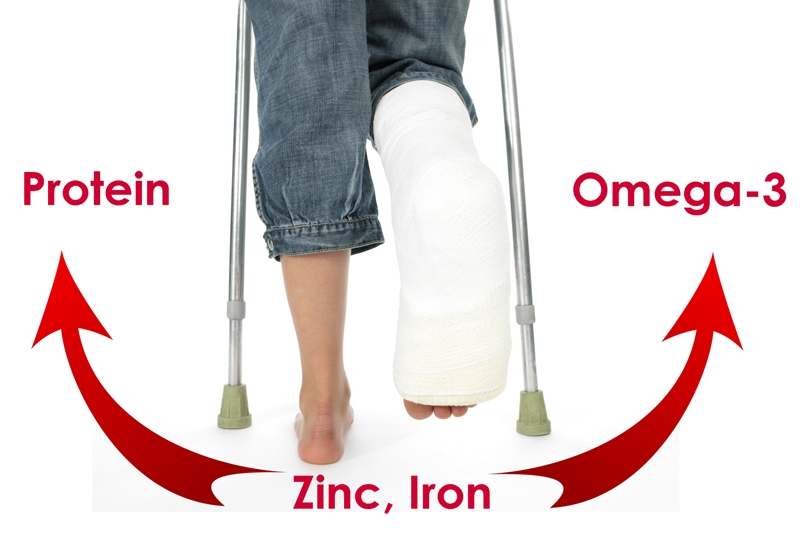
- In the case of the Achilles tendon (the most common tendon affected) it may be difficult to perform plantar flexion of the foot (see figure 2).
- Tendon pain is often bilateral – ie occurs in the same tendon in both left and right limbs. This is a telling sign as it is very rare for an athlete to develop bilateral tendon injuries at the same time.
Figure 2: Plantar flexion

Plantar flexion involves pointing the foot downwards – eg rising up on tip-toes.
Recent evidence
What does the more recent science say about fluoroquinolone use and tendon injury and rupture? In terms of why it happens, compelling evidence suggests that fluoroquinolones can rapidly affect the chemical composition of the tendon structure by depleting levels of compounds known as glycosaminoglycans (GAGs - compounds vital to the elasticity and integrity of structural tissue) in the tendon. This was confirmed by a study in which seven men took 500ms of Ciprofloxacin twice a day for 10 days(11). As figure 3 shows, after ten days, there was a marked reduction in the GAG content of the Achilles tendon, which though reversible, still hadn’t fully recovered five months after ending the Ciprofloxacin course.Figure 3: GAG levels in the Achilles tendon after 10 days of Ciprofloxacin
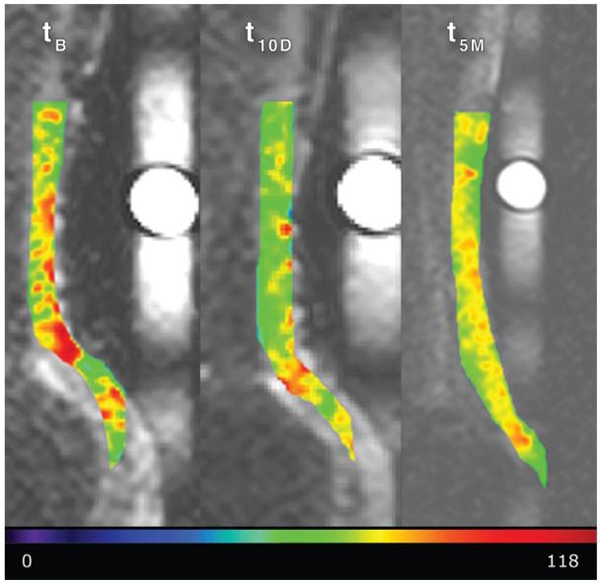
Left = pre-Ciprofloxacin, middle = after 10 days of Ciprofloxacin, right = 5 months later. Red/orange areas indicate high GAG levels in the tendon; green = lower levels.
In another study on mice, researchers looked at tendon healing capacity in those treated with a fluoroquinolone called Fleroxacin before tendon surgery(12). Compared to control mice who received no Fleroxacin, the treated mice showed significantly poorer healing after surgery. Moreover, the treated mice had a significantly reduced tendon cross-sectional area and the researchers concluded that the fluoroquinolone treatment had negatively influenced tendon healing, which could have implications for athletes undergoing tendon surgery/repair in the months following a course of fluoroquinolones.
Relative risk data
Are there certain types of fluoroquinolone antibiotics that are less or more harmful than others? Well, the more recent research has suggested that Ciprofloxacin, Fleroxacin, Pefloxacin and Ofloxacin present the greatest threat to tendon health(13). However, while other fluoroquinolones such as Trovafloxacin and Levofloxacin may present less of a risk, they are not risk free. For example, Levofloxacin has been implicated in Achilles tendon rupture in some case studies(14), while for other fluoroquinolones, there may simply not be enough data to determine safety one way or the other.More worryingly is that the recent evidence suggests that when it comes to tendonitis or tendon rupture, athletes and fitness enthusiasts may be especially vulnerable to the effects of fluoroquinolones. There are a number of reasons why this is the case. Firstly, excessive loading of tendons during physical training is regarded as a major stimulus for tendon degeneration. This is because exercise increases the production of enzymes known as’matrix metalloproteinases’, some of which can adversely alter the structure of the extracellular matrix of tendons(15).
We also know that low-dose corticosteroids in isolation can increase the risk of Achilles tendon rupture, and evidence suggests that combined use of corticosteroids with fluoroquinolones potentiates this adverse effect(16,17). Indeed, studies suggest that over 50% of patients with fluoroquinolone-related tendon rupture had received systemic or inhaled corticosteroids(18), and that patients prescribed both fluoroquinolones and corticosteroids have a 46-fold greater risk of Achilles tendon rupture than those taking neither medication(19)!
Given these facts, a review of fluoroquinolone use among athletes recommended that athletes should NOT be prescribed fluoroquinolones and should be given alternative antibiotics whenever possible(20). This is particularly true in the light of the added risk of corticosteroid treatment; asthma is common among sportsmen and women(21), many of whom may be using corticosteroid medication. Fluoroquinolone use in such athletes could therefore be very hazardous.
When fluoroquinolone antibiotics are the only option for an athlete, there’s some evidence from cell culture studies that taking vitamin E at the same time could help to alleviate some of the harmful effects(22,23). This might occur due to the ability of vitamin E to help prevent of free-radical damage in biological membranes. However, whether this protective effect is significant in humans undergoing fluoroquinolone treatment is unknown and the best option by far is for athletes to avoid fluoroquinolones altogether if possible.
Rehab after fluoroquinolone use
Graduated eccentric training regimes, in which muscle tendons are subjected to increasing loads during the lowering phase of strength training, have proved both popular and effective for treatment and rehab of tendon injuries(24). For sportsmen and women, eccentric training programs have been shown to be particularly effective, resulting in a success rate of around 90% in those with tendinopathy(25) – a significantly better outcome than for the (more sedentary) population as a whole(26).However, while loading tendon with eccentric exercise may be appropriate for treating tendinopathy most athletes, this approach should NOT be used for treating fluoroquinolone-induced tendon conditions, at least in the early stages of symptoms. In study on this topic, researchers concluded that patients with fluoroquinolone-related tendinopathy should be rehabilitated using a 2-phase approach (see box 1)(27):
- An initial phase of bracing and support to allow the tendon to recover from the chemical injury caused by the fluoroquinolone.
- A second phase, consisting of progressive loading.
Box 1: A two-phase approach for rehab of fluoroquinolone-induced tendinopathy
The approach advocated by Green and his colleagues consists of an overlapping 2-phased intervention. The first phase consisted of techniques to protect the tendon from overload stresses, and the second phase consisted of graduated loading of the tendon and muscle. In the early stages of treatment, the tendon is likely to overload easily, causing inflammation. To protect the tendon from overloading forces, techniques should used initially to unload the tendon during weight-bearing activities – eg use of crutches and heel lifts for the purpose of decreasing tendon loading. During the third week of therapy, a counterforce Achilles tendon brace (a non-elastic constraint with a tension strap that crosses the Achilles tendon) can be used during functional weight-bearing activities, excluding specific exercises. The theory behind the tendon brace is that the pressure from the tension strap limits muscle expansion at the time of contraction resulting in decreased stress within the tendon.After three weeks, a progressive exercise program consisting of graduated loading of the tendon begins. The athlete’s feedback in these early stages is important and the progression in loading needs to be very gradual; patients should be encouraged to keep a daily log of exercise performed and their responses to it. Ancillary exercises such as deep water walking, gentle stretching and stationary cycling (with the arch of his foot contacting the pedal to decrease the force on the Achilles tendon) can also be useful. This phase may take three months or more before full functionality is restored.
Summary and recommendations
Over the past two decades, evidence has steadily accumulated suggesting that fluoroquinolone antibiotics are harmful for sportsmen and women, who seem particularly vulnerable to their effects. Not only do they adversely affect the chemical composition and structural integrity of tendons, their use seems to inhibit the normal repair mechanisms that bring about recovery from tendon injury. Worse, the risk of fluoroquinolone-induced tendinopathy is further increased when corticosteroid medication is being used, which is the case in many athletes with asthmatic conditions. In the light of the above, athletes and their coaches/clinicians should follow the recommendations below when athletes have taken a course of fluoroquinolone antibiotics at anytime over the past six months.Practical recommendations
- Athletes should avoid all use of fluoroquinolone antibiotics unless no alternative is available. This is especially true if corticosteroid medication is also used. Athletes should alert their physicians that they train regularly and ask for an alternative antibiotic if possible.
- If no alternative to a fluoroquinolone is available, athletes should immediately reduce high-intensity and ballistic activities and total training volume. These reductions should remain throughout the duration of the antibiotic course. Athletes and their coaches should also be aware of the increased risk for the development of musculoskeletal complications for up to six months following the antibiotic treatment and modify training practices as necessary. Co-administration of vitamin E supplements during the course of antibiotics might provide some protective effect.
- Oral or injectable corticosteroids should NEVER be used or administered while an athlete is taking fluoroquinolones.
- If an athlete has no symptoms after completing the full course of the antibiotic, then a graduated return to full activity under direct medical supervision should be initiated, with close monitoring for the development of musculoskeletal symptoms, particularly tendon aches and pains.
- If any pre-rupture symptoms (see above) are noted, all athletic activity should cease immediately and fluoroquinolone use should be discontinued if possible.
- Sports clinicians and trainers treating fluoroquinolone-induced tendinopathy should be aware that tendons may not respond well to the usual rehab protocols (eg eccentric training), and that an extended period of force unloading may be required before a very gradual program if eccentric training begins.
- Toxicology 2005, 212, 24-36
- Int. J. Antimi- crob. Agents 2010, 35, 366-374
- Antimicrob. Agents Chemother. 2000, 44, 261-266
- Arch. Toxicol. 2001, 75, 97-102
- Arch. Toxicol. 2001, 75, 369-374
- Arch. Toxicol. 2003, 77, 521-526
- Am. J. Sports Med. 2000, 28, 364-369
- Clin Infect Dis. 2003 Jun 1;36(11):1404-10
- US FDA Alert: 7/8/2008 - www.fda.gov/drugs/drugsafety/postmarketdrugsafetyinformationforpatientsandproviders/ucm126085.htm
- J Clin Aesthet Dermatol. 2010 April; 3(4): 49–54
- Radiology. 2015 Jun; 275(3): 763–771
- Am J Sports Med. 2014 Dec;42(12):2851-9
- Biomed Semantics. 2015 May 1;6:18.
- Foot Ankle Int. 2007;28(12):1287–1289; Chemotherapy. 2007;53(2):85–103
- Br J Sports Med. 2005;39(11):789–791
- BMJ Case Rep. 2009;2009. doi:10.1136/bcr.08. 2008.0697
- J Plast Reconstr Aesthet Surg. 2008;61(7):830–834
- Clin Infect Dis. 2003;36(11):1404–1410
- Drug Saf. 2006;29(10):889–896
- J Athl Train 2014;49(3):422–427
- Dan Med J. 2012;59(4):A4405
- BMC Pharmacol. 2008 Feb 11;8:2. doi: 10.1186/1471-2210-8-2
- Hum Exp Toxicol. 2002;21(12):635–641
- Sports Med Arthrosc Rev. 2000;8(1):17–31
- Sports Traumatol Arthrosc. 2003;11(5):327–333
- J Med Sci Sport. 2007;10(1):52–58
- Phys Ther. 2002;82(12):1224–1231
Newsletter Sign Up
Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Keep up with latest sports science research and apply it to maximize performance
Today you have the chance to join a group of athletes, and sports coaches/trainers who all have something special in common...
They use the latest research to improve performance for themselves and their clients - both athletes and sports teams - with help from global specialists in the fields of sports science, sports medicine and sports psychology.
They do this by reading Sports Performance Bulletin, an easy-to-digest but serious-minded journal dedicated to high performance sports. SPB offers a wealth of information and insight into the latest research, in an easily-accessible and understood format, along with a wealth of practical recommendations.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Performance Bulletin helps dedicated endurance athletes improve their performance. Sense-checking the latest sports science research, and sourcing evidence and case studies to support findings, Sports Performance Bulletin turns proven insights into easily digestible practical advice. Supporting athletes, coaches and professionals who wish to ensure their guidance and programmes are kept right up to date and based on credible science.