You are viewing 1 of your 1 free articles. For unlimited access take a risk-free trial
Mental illness in athletes: the most hidden injury?

In the first of a 2-part article, Andrew Hamilton looks at the incidence of depression and anxiety disorders in competitive sport, and what the science says about the best treatment approaches
The traditional image of athletes is one of physical prowess and extreme mental toughness – hardened to the pressures of training and competition. It’s hardly surprising therefore that the issue of mental health in athletes is not exactly top of the sports health agenda. After all, surely athletes are better psychologically equipped to withstand the stresses and strains of modern life than the average couch potato? And anyway, we already know from previous research that regular vigorous exercise is a useful tool for combating depression. For example, one meta-study (a study that pools data from a number of prior studies in the same area) looked at the outcomes of 1101 participants in 28 different studies and found that exercise produced a ‘moderate clinical’ effect in the treatment of depression(1).Athletes are equally vulnerable
Given the facts above it’s natural to assume that a) because of their ‘tough personalities’, athletes are less likely to succumb to mental illness and b) those who might be prone to mental illness are protected to a degree by their high levels of physical activity. Unfortunately however, the reality is far less clear. A 2011 French study examined the psychological health of more than 2,000 elite athletes(2). In particular, it aimed to identify the principal psychological problems (see panel 1 below) encountered within French elite athletes, and the variations in prevalence according to gender and the sport practiced (see figure 1). The sample used in this study was very comprehensive as it represented 13% of the country’s elite athletes at the time. The main findings were as follows:- *17% of the athletes had a current or recent psychopathology (eg anxiety, eating disorders, depression, sleep problems etc) at the time of their evaluation, with generalised anxiety disorder being the most prevalent at 6%.
- *Women were a third more likely than men to have a current or recent psychopathology (20.2% of women vs. 15.1% of men).
- *Female athletes were 56% more likely than males to have suffered from anxiety disorders over their lifetime.
- *Significantly higher rates of anxiety disorders (around 4 times higher in women and 3 times higher in men) were found in aesthetic sports such as gymnastics, synchronised swimming and figure skating.
Figure 1: Lifetime prevalence (%) of minor or major depression by type of sport practiced
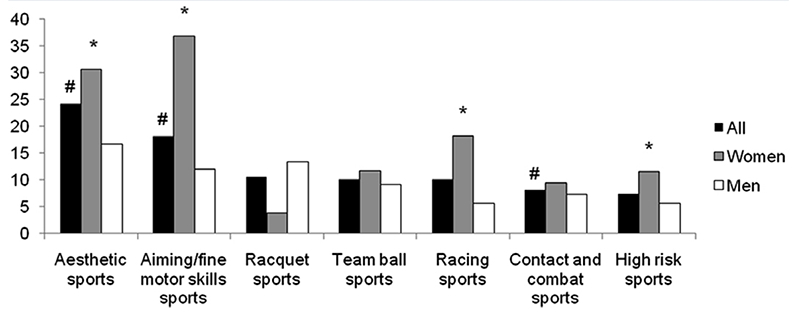
NB: # = significant difference with all other sports. * = significant difference between men and women
It’s important to note that the prevalence of this type of psychological condition in this (large) sample of athletes was similar to that found in the general population at large. For example, a study into the prevalence of anxiety disorders in French adults published the same year found that the overall prevalence of anxiety disorders was estimated to be 21.6%, with generalised anxiety disorder being most prevalent (12.8%)(3).
Given that this study only looked for anxiety disorders in the general population and in the athlete study, 61% of the athletes studied were seen by psychologists and 38% by physicians (which probably resulted in lower rates of psychopathology than would have been reported by psychologists only), we can be pretty confident that athletes are by no means immune from mental conditions such as anxiety disorders and are no different from the general population in this respect. This seems to be further confirmed by the fact that the difference in anxiety scores observed in male and female athletes closely mirrored those in the population at large.
Panel 1: Classifying psychological/mental health disorders
There are numerous types of psychological disorders reported in the literature. Some of the most common are as follows:- *Anxiety disorders – characterised by a diffuse, extremely unpleasant feeling of vulnerability, apprehension, and fear. Symptoms of anxiety disorders include motor tension (trembling, jumpiness, inability to relax), hyperactivity (racing heart, dizziness, perspiration), and apprehension (disturbing thoughts). While the causes of anxiety disorders are not completely understood, it is generally believed that some of the disorders (such as specific phobias, obsessive-compulsive disorders, and panic disorders) may have a genetic basis. One cause may be the inadequate action of the neurotransmitter gamma-aminobutyric acid (GABA).
- *Mood disorders - characterised primarily by a disturbance in mood (although all psychological disorders affect mood). In major depressive disorder, a person, for no apparent reason, experiences at least two or more weeks of depressed moods, feelings of worthlessness, and diminished interest or pleasure in most activities. To be classified as a major depressive disorder, the episode must be accompanied by clinically significant distress and impairment in social, occupational, or other areas of daily living. In a bipolar disorder, a person alternates between the hopelessness and lethargy of depression and the overexcited state of mania. Mania is manifested by hyperactivity and wild excitement. A person suffering from this disorder may lose control and act very inappropriately and sometimes destructively.
- *Schizophrenia and other psychotic disorders - severe disorders characterised by distorted thoughts and perceptions, atypical communication, inappropriate emotion, abnormal motor behaviour, and social withdrawal. The slow-developing schizophrenia known as chronic or process schizophrenia has a poor prognosis for recovery. However, when a formerly well-adjusted individual develops schizophrenia (known as reactive or acute schizophrenia), there is a better chance of recovery.
- *Eating disorders - characterised by severe disturbances in eating behaviour. Anorexia nervosa is characterised by a refusal to maintain a minimally normal weight, intense fear of gaining weight, and distortion in the perception of the shape or size of one's body. Postmenarcheal females with this condition are often amenorrheic (having missed three consecutive menstrual cycles). Muscular weakness and osteoporosis (bone loss) may also occur. Bulimia nervosa is manifested by binge eating and use of inappropriate techniques, such as purging or use of laxatives, to prevent weight gain. To qualify for this diagnosis, an individual must engage in binge eating and the inappropriate compensatory acts (purging, use of laxatives), on average, twice a week for three months.
Is athletic competition a risk factor?
In the light of the findings on the incidence of mental illness in athletes above(2), it’s natural to speculate whether athletes are actually more susceptible – for example, as a result of the stresses and strains of competition or just by virtue of the fact that successful athletes tend to be quite ‘driven’ and therefore set themselves higher standards with commensurate levels of expectation and the pressure to perform.Once again however, there’s no evidence to suggest that athletes are significantly different to the average sedentary adult in this respect. In one study, Swiss researchers looked at whether participation in elite sport interacted with stress in decreasing or increasing symptoms of depression and anxiety among adolescents(4). In addition, they also investigated whether the interplay between participation in high-performance sport and stress was related to the perceived quality of sleep. To do this, 434 adolescents (278 girls, 156 boys) from fifteen Swiss Olympic Sport Classes and nine conventional classes answered a questionnaire and completed a 7-day sleep log.
The results showed (unsurprisingly) that increased stress was related to more depressive symptoms and higher scores for trait-anxiety. Moreover, those classified as having poor sleep also reported higher levels of depressive symptoms. Interestingly however, the researchers found that competing at elite level did not affect the risk of depression, and they concluded that while high-level sport participation didn’t seem to act as a ‘stress buffer’, it wasn’t found to be an additional source of distress for adolescents.
Is competition good?
Further evidence supporting the notion that competition isn’t a risk factor for mental disorders in athletes comes from a Spanish study, which looked at direct and indirect relationships among self-motivation, perceived competition and psychological well-being and ill-being in athletes(5). Data from 491 Spanish college students involved in competitive sports were collected following which statistical analyses were carried out. Contrary to the notion that competition induced mental disorder, the researchers discovered that the higher levels of competition perceived by the athletes, the lower the incidence of mental disorder and the higher the level of well-being.That generalised anxiety appears to the most prevalent disorder in both male and female athletes is perhaps not surprising. Many competitive athletes are in adolescence and early adulthood – exactly the age range where the highest rates of anxiety are recorded among the population as a whole. Just as unsatisfactory school performance is often a source of anxiety in adolescents, it is easily conceivable that the pressure to excel within their sport could present a risk factor in high level athletes; especially if a large discrepancy exists between the desired or imposed goals and actual performance, and thus becomes a source of excessive worry. Yet despite the pressures inherent to high level sport, the overall prevalence of generalised anxiety in athletes appears no higher than in the overall population.
Major depression and elite sport
In a large study, researchers found that in the general population, the lifetime prevalence of major depression (bipolar depression, schizophrenia etc.) was 12.8% (ie a 1 in 8 chance of an individual having succumbed), with the greatest rates found in 18 to 24 year olds(6). However, the results of the French study on athletes above(2) indicate that less than 1% of athletes in the (large) sample were suffering from major depression within the six months leading up to their evaluation, with a rate of 2.6% over a whole lifetime.Even though it’s difficult to compare the prevalence of depression across population studies, the tremendous difference between that found within this sample population and those of the greater population at large is noteworthy and encouraging for high level sport. Elite athletes are frequently characterised as being strongly optimistic and able to adapt and even thrive under pressure. As researchers are determining which genes may confer physiological advantages to elite athletes, the same concept may be relevant for psychological resilience, especially as gene polymorphisms have been identified which confer either resilience or vulnerability to stress, fear, and in turn, the development of depression. In plain English, it may be that competitive athletes are more likely to be genetically 'hard wired' in a way that makes them less likely to succumb to major depression.
The riskiest sports and best routes to recovery
So far, we have seen that while elite athletes may be less at risk from severe mental illnesses such as schizophrenia and bipolar depression, the prevalence of other types of mental illness is just as high in athletes as in the population at large. In the second part of this article, we'll investigate which sports are most associated with mental illness, the best management and treatment options are for athletes in need of help and the implications for coaches and clinicians with athletes in their care.References
- Cochrane Database Syst Rev. 2012 Jul 11;7:CD004366
- PLoS ONE 2011; 6(5): e19007. doi:10.1371/journal.pone.0019007
- Eur Psychiatry. 2011 Sep;26(6):339-45
- Percept Mot Skills. 2011 Apr;112(2):581-99
- Salud Publica Mex. 2010 Nov-Dec;52(6):517-23
- Acta Psychiatr Scand Suppl.2004; pp 21–27
Newsletter Sign Up
Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Editor's Picks
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Keep up with latest sports science research and apply it to maximize performance
Today you have the chance to join a group of athletes, and sports coaches/trainers who all have something special in common...
They use the latest research to improve performance for themselves and their clients - both athletes and sports teams - with help from global specialists in the fields of sports science, sports medicine and sports psychology.
They do this by reading Sports Performance Bulletin, an easy-to-digest but serious-minded journal dedicated to high performance sports. SPB offers a wealth of information and insight into the latest research, in an easily-accessible and understood format, along with a wealth of practical recommendations.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Performance Bulletin helps dedicated endurance athletes improve their performance. Sense-checking the latest sports science research, and sourcing evidence and case studies to support findings, Sports Performance Bulletin turns proven insights into easily digestible practical advice. Supporting athletes, coaches and professionals who wish to ensure their guidance and programmes are kept right up to date and based on credible science.











