You are viewing 1 of your 1 free articles. For unlimited access take a risk-free trial
Bug off! keeping illness at bay with probiotics
With winter upon us, the risk of coming down with coughs, colds and flu is a real concern for athletes. With that in mind, Andrew Hamilton asks whether the use of probiotic supplements can boost your immunity and help keep your training on track...
Andrew Hamilton asks whether the use of probiotic supplements can boost your immunity and help keep your training on track...
As we head towards winter, with colder weather and dark nights, many endurance athletes will take the opportunity to wind down the training a little and recuperate, which is no bad thing. But this doesn’t mean ceasing training completely – after all, the more of the previous season’s hard-earned fitness that slips away, the longer the haul back to full fitness next season! This is also a time when the old adage ‘a change is as good as a rest’ is relevant. Many athletes will want to use this time working on different aspects of fitness such as strength, which are simply not possible to squeeze in during the competition season.
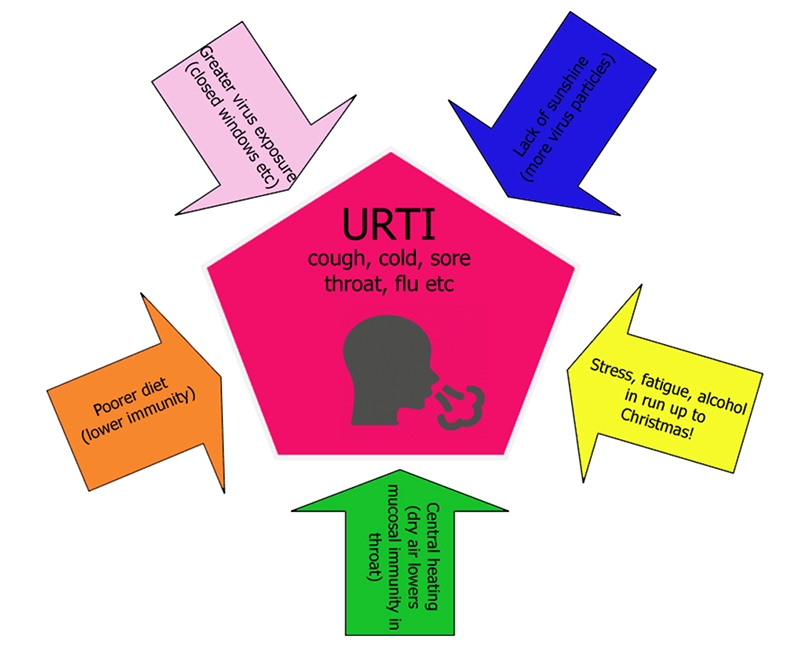
Either way, what nobody wants is to succumb to illnesses such as colds, coughs, sore throats or even influenza. Yet for all sorts of reasons, this is the time of year when your training is most likely to be scuppered by these kinds of upper respiratory tract infections (URTIs). Lack of strong sunlight (which kills cold viruses) means there are more viruses around. Colder weather, with office windows more likely to be shut, means that these viruses can circulate more easily. Together with poorer nutritional habits in the winter, this explains the surge in URTIs during the winter months (see figure 1).
Figure 1: Winter risk of urtis
Defences
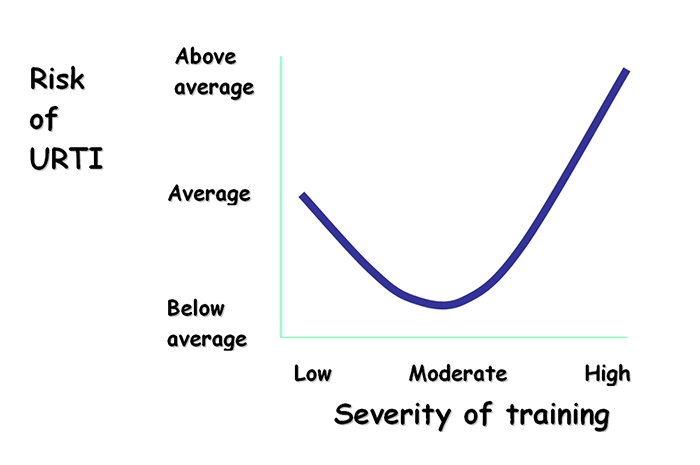
Each and every day (winter or not), you will likely encounter numerous viruses (and potentially infectious bacteria). However, the good news is that the human body is equipped with an amazing immune system, which can defend the body against most attacks. Even better for athletes, numerous studies have indicated that higher levels of fitness are associated with enhanced immunity, which means that if you’re fit, you’re less likely to succumb to an URTI. The caveat however is that high training loads can LOWER your immunity, which means you’re more likely to become ill. This fitness/training load relationship with immunity is described as a J-shaped immunity curve (see figure 2).
Training load isn’t the only thing that affects your immunity and the ability to fight off infection. Lifestyle factors such as stress and nutrition are important too. Stress, especially over prolonged periods of time, is known to lower immunityImmunol Res. 2014 May;58(2-3):193-210. However, it’s not always possible to avoid periods of stress, which is why, over the years, many researchers have focused extensively on nutrition and immunity.
Because of the complexity and sophistication of the human immune system, even small deficits in nutritional status are capable of affecting your immunityTher Umsch. 2014 Jan;71(1):55-61. A number of nutrients have attracted special interest in this respect, including zinc, selenium, iron, copper, and the vitamins A, C, E, B6 and folic acidAm J Clin Nutr. 1997 Aug;66(2):460S-463S. In more recent years however, probiotic supplements and drinks (see box 1) have been extensively investigated for their potential immune-enhancing properties.
BOX 1: WHAT ARE PROBIOTICS?
The term ‘probiotic’ refers to dietary supplements (tablets, capsules, powders, lozenges and gums) and foods (such as yogurt and other fermented products) that contain beneficial or friendly bacteria. The organisms themselves are also called probiotics. These beneficial bacteria have a twofold function; by crowding out harmful bacteria, they can prevent harmful illness-producing pathogens from accumulating in the gut. Secondly, probiotics are involved in some aspects of normal gut metabolism – for example the synthesis of some vitamins and hormones.
There are many general types of bacteria used in probiotic products (two common ones are Lactobacillus and Bifidobacterium), and many different species as well as strains within species. They have different physiological effects—and thus possibly different health benefits (as well as possible risks). Some yeasts such as Saccharmyces, can also act as probiotics. Probiotic products may contain a single strain or many strains, and the number of organisms in a daily dose can range from 1 billion to more than 250 billion. Many manufacturers boast that their products contain unique probiotics and/ or combinations of strains that make them even better for you—and often charge a premium price!
Figure 2: The J-shaped immunity curve
Evidence for probiotics
Of all the functional foods that claim to enhance health and performance, probiotics - in both drink and tablet/capsule form- are perhaps the most popular. Indeed, recent market analysis shows that around the globe over £20billion is spent on these products annually! But how effective are they for otherwise healthy people, and are they useful for athletic performance?
During the last fifteen years, there’s been an explosion of research into the immune boosting properties of probiotics and the results have been very encouraging. What’s been lacking until more recently however is good placebo-controlled randomised trials carried out in the field – ie on athletes engaged in their normal training programmes. To complicate matters further, numerous strains of probiotic bacteria have been used in studies, some of which may be far less effective than others. This all makes it difficult to determine just how effective probiotic supplementation for someone in hard training really is!
A 2013 study looked at the effects of probiotic supplementation on the duration, incidence and severity of infections in 30 elite rugby union players who took a supplement for 4 weeksJ Sci Med Sport. 2013 Aug 30. pii: S1440-2440(13)00190-4). During the probiotic treatment 14/30 participants never experienced a single upper respiratory tract illness or gastrointestinal episode, compared to 6/30 on the placebo supplementation (a scientifically significant reduction). Also, the number of days of illness tended to be less when the probiotic was taken.
Another study looked at Lactobacillus fermentum supplementation and gastrointestinal and respiratory-tract illness symptoms in 99 competitive cyclistsNutr J. 2011 Apr 11;10:30). The cyclists were randomised to either probiotic (a minimum of 1 billion Lactobacillus fermentum CFUs per day) or placebo treatment for 11 weeks in a ‘double-blind, randomised, controlled’ trial – the most rigorous kind of scientific trial. At higher training loads, there was an average 70% reduction in the severity of gastrointestinal illness, which became more pronounced as training load increased. Also, the duration and severity of upper respiratory-tract illness symptoms was reduced by around 30%.
In another double-blind, placebo-controlled cross over trial study, scientists investigated the use of Lactobacillus fermentum in 20 elite male runners over a 4-month winter training seasonBr J Sports Med. 2010 Mar;44(4):222-6). Athletes taking the probiotic supplement reported less than half the number of days of respiratory symptoms during the supplementation period (30 days) compared with the placebo group (72 days). Reported illness severity was also lower for episodes occurring during the supplementation period.
In a further recent study, 84 athletes took either a placebo or probiotic supplement (Lactobacillus casei Shirota) for 4 monthsInt J Sport Nutr Exerc Metab. 2011 Feb;21(1):55-64). The athletes taking the probiotic experienced significantly less URTIs than those who didn’t. However, to illustrate that not all probiotics are created equal, the same scientists investigated the effect of another probiotic (Lactobacillus salivarius) on infection, cold symptom duration and severity, and immunity in 66 endurance athletes. They found that it didn’t reduce the frequency of URTIsInt J Sport Nutr Exerc Metab. 2012 Aug;22(4):235-42). In other words, it seems that if you’re tempted to use probiotics, you should try a strain for which there is good evidence in the scientific literature.
Stock up the fridge?
At this point, you’re probably thinking “Great – time to stock up the fridge with probiotic drinks!” However, while these studies make for encouraging reading, there are still some doubts about probiotic use. This is partly because in these studies, numerous strains of probiotic bacteria have been used, some of which may be far less effective than others. There’s also the issue of how fresh or ‘viable’ a probiotic supplement is and how resistant it is to degradation by naturally produced acid in the stomach (see box 2).
BOX 2: HOW VIABLE IS YOUR PROBIOTIC?
To be effective and therapeutic, probiotics have to be able to deliver a sufficient amount of the friendly bacteria they contain to the small intestine. Simply swallowing enough active bacteria is no guarantee, especially when faced with the very acidic conditions of the stomach, which the bacteria need to pass through before they can enter the small intestine.
With this in mind, scientists at University College London have carried out research on the viability of solid and liquid probiotic formulationsBeneficial Microbes 2015, Vol. 6, No. 1, pp. 141-151. They looked at a probiotic called lactobacillis bacteria, which is found in a number of popular products on the supermarket shelves. In particular, the study was designed to mimic the challenges faced during oral delivery. These were:
- Did the product provide the stated number of viable bacteria as per the labels claimed?
- Could the bacteria survive exposure to stomach acid?
- Could the bacteria thrive upon arrival in the gut?
The researchers compared 8 commercially available products. The good news was that the liquid products (such as yoghurts and probiotic drinks) all contained viable bacteria equal to or more than the claimed amounts on the labels. This was in contrast to solid probiotics (capsules etc), which all contained fewer viable bacteria than the labels claimed.
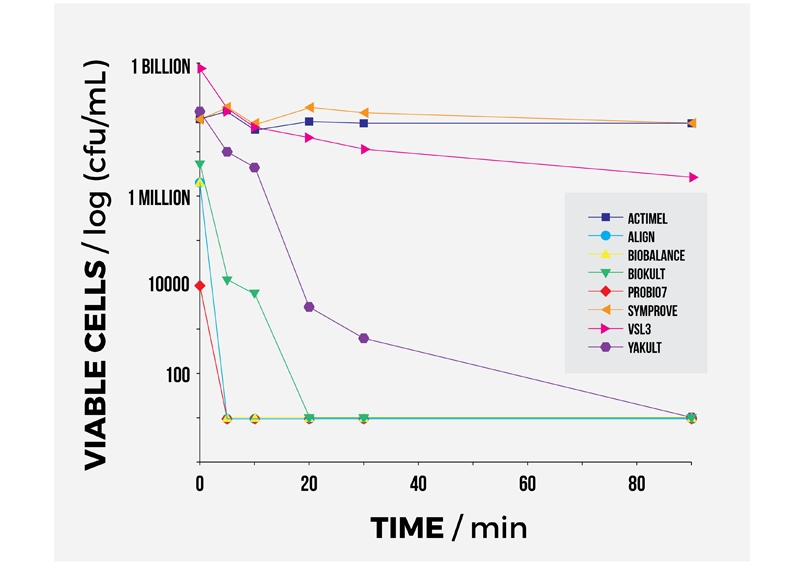
However, regardless of whether they were supplied in liquid or solid form, all the products lost viable bacteria when exposed to the acidic gastric fluid. Despite this, three of the products (Actimel, VSL3 and Symprove) maintained viable bacterial numbers for up 90 minutes after exposure to stomach acid (see figure 3 below). This suggests that these products might be able to deliver useful amounts of bacteria to the small intestine of the gut, which is where they are able to deliver any potential benefits. An important implication of these findings is that any probiotic should be taken on an empty tummy and at least 15 minutes before food. This is because in these conditions, gastric emptying time will be faster, meaning less exposure of the bacteria to destructive tummy acid.
Figure 3: Probiotic viability after exposure to stomach acid
To help us come to a conclusion, it’s worth considering a couple of review studies (studies that pool together all the data from previous studies) into the benefits of probiotics. The first was carried out last year by Chinese researchersCochrane Database Syst Rev. 2015 Feb 3;2:CD006895. It concluded that probiotics did seem to reduce the number of participants experiencing episodes of an acute URTI, the mean duration of an episode of acute URTI, antibiotic use and cold-related school absence, and that probiotic use could be more beneficial than nothing. However, it also concluded that because of all the confounding variables such as the type of probiotic used, viability (see box 2), the probiotic quantity, length of supplementation etc, it was difficult to determine just how effective probiotic supplementation really was. However, another review study on probiotic use and URTIs, also published last year, provides further evidence that probiotics could be usefulGlob Adv Health Med. 2015 Nov; 4(6): 18–19. The individual studies reviewed and the findings are summarised in table 1.
Table 1 Effects of probiotics after 3 to 8 months of treatment 2022 10 04
| What was measured | Without probiotics | With probiotics | Quality of the evidence | Conclusion |
|---|---|---|---|---|
| Number of people who had at least 1 URTI (7 studies, 1927 people) | 30 out of 100 | 19 out of 100 (from 14 to 25) | moderate | Probiotics probably reduce the number of people with a URTI. |
| Number of URTI per person in 1 y (5 studies, 1608 people) | 4 URTI per person per y | 1 URTI fewer | low | Probiotics may reduce the number of URTIs a person has per year. |
| Duration of URTI (3 studies, 831 people) | 7 d | 2 d fewer | moderate | Probiotics probably reduce how long the URTI lasts. |
| Number of people needing time off from school or work (1 study, 80 people) | 35 out of 100 | 5 out of 100 (from 1 to 20) | very low | It is uncertain whether the number of people needing time off is reduced with probiotics. |
| Number of people prescribed antibiotics (4 studies, 1184 people) | 20 out of 100 | 13 out of 100 (from 9 to 19) | low | Probiotics may reduce the number of people prescribed antibiotics. |
| Side effects (4 studies, 1234 people) | 10 out of 100 | low | Probiotics may have little to no effect on side effects. |
Summary and practical advice
Given the most up-to-date evidence, what can we conclude about the use of probiotics? Well, on balance, it seems that they might be able to deliver some health benefits to anyone in hard training – mainly in terms of supporting immunity and helping to fend off URTIs. But due to the wide range of bacteria used in these different studies and the problems in getting enough of the right bacteria through the stomach and into the gut, it’s by no means guaranteed that everyone will see tangible benefits from probiotic supplementation. However, the balance of evidence suggests that used correctly, and in conjunction with other measures, probiotics could make you less susceptible to illness and infection. With that in mind, the practical tips box below provides a range of suggestions to help keep you well this winter!
PRACTICAL ADVICE
No simple supplement on its own will keep you cough, cold and flu free. However, by sticking to the guidelines below, you can significantly minimise your risk of contracting an URTI this winter.
1. Day-to-day nutrition
At the heart of any strategy to maintain and maximise immunity is a healthy lifestyle. This involves eating a healthy diet, which should contain:
- Plenty of fresh fruits and vegetables, which play a vital role in promoting long-term health;
- Ample wholegrain carbohydrates (eg wholegrain breads, rice, cereals and pasta etc) to support training;
- Sufficient high-quality, proteins (eg fresh fish, lean meats, nuts and seeds, beans, peas and lentils) to support recovery.
- Plenty of fluid to help hydrate during and after exercise;
- Only small amounts of sugary or processed (and often fatty) foods, which have little nutritional value and may actually disturb some aspects of the body’s metabolism.
2. Lifestyle
The following lifestyle strategies can also help boost immunity and reduce exposure to pathogens:
- Get plenty of sleep and try to stick to regular hours (disturbances to your body clock can temporarily reduce immunity).
- Avoid (wherever possible) day-today stress, which can also lower immune function.
- Consume alcohol in moderation only as excessive consumption can suppress immunity.
- Maintain good hygiene at all times. Regular hand washing is especially important after contact with shared surfaces (eg after using the gym, handling a petrol pump when filling the car, using door handles in busy public places etc)
3. Training
- Be mindful of the J-shaped immunity curve. Refrain from sustained, heavy periods of training, which can markedly reduce immune function.
- If you’re feeling at all under the weather, don’t be afraid to take a couple of days off – it could save you a couple of weeks off down the line!
- Never conduct low-carbohydrate training(which lowers immune function) when you’re feeling under the weather.
- Help minimise the temporary post exercise dip in immunity by consuming a recovery drink containing protein and carbohydrate immediately after training.
4. Probiotics
The balance of evidence suggests that probiotic supplementation can reduce both the incidence and severity of URTIs, as well as providing gastrointestinal health benefits:
- If you use probiotics, stick to bacteria strains that have proven to be effective in studies such as Lactobacillus fermentum and Lactobacillus casei.
- Probiotics in liquid form are more likely to be effective than dried forms such as capsules.
- Take any probiotic on an empty tummy and at least 15 minutes before food. A good time is soon after rising in the morning, but before breakfast.
- Bear in mind that beneficial changes in gut flora from probiotic take time to accrue, which means that probiotics are not a ‘quick fix’ for boosting immunity.
- Probiotics are definitely recommended following a course of antibiotic treatment.
Newsletter Sign Up
Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Editor's Picks
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Keep up with latest sports science research and apply it to maximize performance
Today you have the chance to join a group of athletes, and sports coaches/trainers who all have something special in common...
They use the latest research to improve performance for themselves and their clients - both athletes and sports teams - with help from global specialists in the fields of sports science, sports medicine and sports psychology.
They do this by reading Sports Performance Bulletin, an easy-to-digest but serious-minded journal dedicated to high performance sports. SPB offers a wealth of information and insight into the latest research, in an easily-accessible and understood format, along with a wealth of practical recommendations.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Performance Bulletin helps dedicated endurance athletes improve their performance. Sense-checking the latest sports science research, and sourcing evidence and case studies to support findings, Sports Performance Bulletin turns proven insights into easily digestible practical advice. Supporting athletes, coaches and professionals who wish to ensure their guidance and programmes are kept right up to date and based on credible science.