You are viewing 1 of your 1 free articles. For unlimited access take a risk-free trial
Post-exercise muscle soreness: should you pop pills?
SPB looks at new research into anti-inflammatory medications such as Ibuprofen – specifically whether they really do help speed recovery and combat post-exercise muscle soreness
All athletes in serious training will have experienced (DOMS) delayed-onset muscle soreness at some point. DOMS is an inevitable consequence of unaccustomed, unusually hard or unusually lengthy bouts of exercise, which produce more muscle damage than usual. This muscle damage results in increased levels of inflammation as the body attempts to heal micro-tears in the muscle fibres, and it’s this inflammation that leads to post-exercise soreness. Thus, exercise-induced inflammation is a double-edged sword; although it’s necessary for recovery and training adaptation, it can also produce muscle soreness.
Inflammation, healing and training adaptation
DOMS is a normal and healthy response to hard/long bouts of exercise. Not only does it signify muscle fibers that are healing and adapting to become stronger and more resilient for future training sessions, DOMS also provides a self-limiting mechanism; when muscles are feeling sore and tired, athletes are less inclined or able to train them hard, which ensures that they get the recovery and rest they need!
While DOMS is a normal response to unusually challenging exercise sessions, it is nevertheless frustrating for athletes, especially those seeking to get some high-quality sessions in the run up to a competitive phase. For older athletes in particular, DOMS can be a right pain (literally) because many older athletes report that slowed recovery and greater levels of muscle soreness tend to increase as the years tick by.
There’s hard evidence for this in the literature; an Australian study compared eighteen well-trained cyclists - nine ‘veterans’, average age 45yrs and nine ‘young’ cyclists, average age 24yrs – who all performed three consecutive days of high-intensity 30-minute cycling time trials intended to induce fatigue and decreased performance(1). Each day, before, during, and after each time trial, the cyclists’ perceptions of muscle soreness, fatigue, and recovery were all recorded. Although there was no change in time-trial performance over the three days for either group, muscle soreness and perceived recovery changed significantly (for the worse) over the three days in the veteran group, but not in the young group.
Beating DOMs with anti-inflammatories
Since DOMS occurs primarily as the result of inflammatory responses in muscles, the obvious question is whether DOMS can be ameliorated and recovery from soreness accelerated by the use of over-the-counter non-steroidal anti-inflammatory (NSAID) medications such as Ibuprofen, aspirin, or prescribed NSAID anti-inflammatories such as COX-1(eg Flurbiprofen) and COX-2 (eg Celecoxib) inhibitors (see this article for an explanation of how these NSAID anti-inflammatories work). The logical assumption is that they can help, and this almost certainly explains their popularity among athletes.
The data shows that NSAID medications are often used by athletes to reduce soreness or decrease recovery time after exercise(2,3). Indeed, self-reported NSAID use by collegiate athletes shows that 25 % of females and 20 % of males regularly use NSAIDs to relieve DOMS or to prevent DOMS from occurring(4). But it’s not just elite or club-levels athletes who resort to frequent NSAID use. Data shows that 36 % of recreationally trained college-aged students have reported analgesic use for exercise-associated pain(5), while NSAID usage in the active duty US military is also reported to be extremely common(6).
To put some flesh on the bones with an example, a 2017 study looked at NSAID use among 238 participants at the Ultra Mallorca Serra de Tramuntana (Mallorca, Spain) - an ultra-endurance mountain event, with runners participating either in a 112km ultra, a 67km trail, or a 44km marathon competition(7) Among the study participants, 48.3% reported taking NSAIDs at least for one of the time-points considered: before, during and/or immediately after the competition, with more positive responses (having taken medication) found for the ultra runners (60.3%) than for the trail runners (49.2%) or the marathon runners (35.5%).
Another 2017 study, this time by Czech scientists, investigated the prevalence of NSAID consumption immediately before, during and immediately after a 24-hour mountain bike race and compared NSAID consumption in two different MTB competitions and across 131 competitors(8). Using questionnaires administered to all the competitors, no less than 10% had consumed NSAID medication at least once during the competition day (immediately before, during or immediately after the race).
Of these, half of the competitors had consumed NSAID after the race – presumably to try and reduce the degree of subsequent DOMS. Interestingly, the average age of NSAID users was significantly higher than non users, lending support to the notion outlined above that older athletes are more likely to suffer from DOMS. In yet another study – this time of 76,654 half-marathon and marathon runners – no less than 12.2% reported regularly using analgesic/anti-inflammatory medication before or during races(9).
Drawbacks of NSAIDs
If NSAID use can help ameliorate DOMS and speed up recovery, their use must be a good thing, right? Unfortunately, it’s not as simple as that as regular NSAID use carries the risk of undesirable side effects, particularly to the gut and digestive system. There’s also evidence that NSAID use can slow down the healing process following a muscle(10) or bone(11,12) injury, and could also increase the risk of kidney injury, especially during long-distance events(13).
A particular potential problem for sportsmen and women who use NSAIDs is the fact that many of these drugs can play havoc with the delicate lining of the stomach, with the potential to cause such serious gastric problems as ulcers gastric bleeding. These risks are not insignificant: one study showed that in the USA, NSAIDs caused more deaths than bone marrow cancers, asthma, cervical cancer or Hodgkin’s disease (cancer of the lymphatic tissues(14). Another study found that on average, one in every 1,200 patients taking NSAIDs for at least two months was likely to die from gastro-intestinal complications – people who would not have died if they had not taken NSAIDs(15). Worryingly for older athletes (who may be more tempted to use NSAIDs), a large UK study also showed that the risk of NSAID-induced gastric bleeding increases rapidly with age, as does death from subsequent complications(16).
Blunting training adaptations
While the absolute risk of irregular NSAID use may not be a major concern for younger athletes, there’s another reason why using NSAIDs in conjunction with training is undesirable. As mentioned above, inflammatory processes are an essential part of remodelling muscle tissue and training adaptation. Excessively dampening down this process could therefore inhibit training adaptation. Indeed, research has found that by blunting the inflammatory response, NSAID use before or immediately after exercise can interfere with training induced adaptations gains(17). In a nutshell, if you regularly use NSAIDs such as ibuprofen before and/or after training, you may not be deriving the full benefits of a training program as your body may fail to properly adapt to the training stimulus.
Do NSAIDs even work?
When deciding whether to use any medicine or medical treatment, medical ethics means that doctors should fully inform patients of the ‘risk-benefit’ equation. This equation basically compares the potential benefits of a medicine or treatment to its risks for that particular user, who can then make a decision as to whether the likely benefits sufficiently outweigh those risks.
In the case of athletes using NSAID medications without advice from a physician, athletes need to inform themselves of how much reduction in DOMS they are likely to experience and whether this reduction is worth the potential downsides of NSAID use. Most athletes who routinely use NSAIDs to minimize DOMS assume that the benefits are very significant (because otherwise they wouldn’t use them). But is this actually true? This question really matters because if the benefits of NSAIDs are minimal or non-existent, the potential side-effects of NSAID use would mean they should not be used in any circumstances.
Alarmingly, when you examine the data from studies on this topic, it’s clear that there is a lot of conflicting and confusing data on just how effective NSAIDs are for reducing DOMS. For instance, researchers found that the prophylactic use of Flurbiprofen was ineffective in reducing delayed-onset muscle soreness (DOMS) following a regimen of seven sets of 10 repetitions of drop jumps executed by trained athletes(18). Conversely, a study using ibuprofen found NSAID treatment enhanced maximal isometric force after a strenuous training session compared to a placebo, but did not influence muscle soreness(19). In a similar vein, a fairly recent study using Ibuprofen found that while NSAID treatment enhanced maximal isometric force after a strenuous training session, it did nothing to reduce DOMS(20).
By contrast, one study suggested that Ibuprofen prior to intense exercise may reduce DOMS, possibly helping improve subsequent exercise performance(21), while another meta-analysis study (one that pools data from a number of previous studies) found that DOMS and subsequent muscular performance might be improved by Ibuprofen in patients recovering from a previous injury(22). However, just to illustrate the uncertainty, a different high-quality and recent meta-analysis study found that NSAIDs do NOT influence performance or muscle soreness in exercise interventions(23)!
New research
These mixed results on NSAIDs and DOMS reduction are perhaps not what we’d expect, so why is there confusion? There are a number of possible explanations: firstly, different NSAIDs target different inflammation pathways in the body (COX1, COX2 or both); secondly, the doses and timings used in the studies are quite variable; thirdly, individuality may play a role (some people react more positively one type of NSAID over another- eg aspirin vs. Ibuprofen.
To try and clear up the confusion, a brand new study on NSAIDs, DOMs and recovery has just been published in the Journal of Science and Medicine in Sport(24). Carried out by the US Army Research Institute of Environmental Medicine, this study was designed to compare the effects of three NSAIDs on muscle soreness and performance vs. a completely inert placebo following a plyometric training session on a leg press device. These NSAIDs were:
· A COX-1 inhibitor (Flurbiprofen)
· ACOX-2 inhibitor (Celecoxib)
· A non-selective (ie COX-1 & COX-2) inhibitor (Ibuprofen)
What they did
On four separate mornings (spaced a week apart) in a completely randomised order, 12 healthy men and women, all of whom were exercising vigorously at least twice per week performed four different trials. Each trial consisted of a performed a single bout of plyometric exercise at 40 % of their 1RM on a plyo-leg press, which was designed to induce muscle damage and soreness. This device is a modified leg press machine in which participants lay on a sled, which rolls back and forth along a track as participants push off of a stationary platform. The advantage of this device is that plyometrics loadings can be precisely controlled and standardized for all participants. The actual exercise consisted of ten sets of ten jumps at a rate of approximately one jump per second for each jump phase.
All four trials were identical apart from what was taken prior to the trial:
· 800 mg Ibuprofen
· 200 mg Celecoxib
· 100 mg Flurbiprofen
· An inert placebo
Immediately after NSAID or placebo ingestion, participants consumed a light breakfast of approximately 8 kcal/kg body weight (60–65 % carbohydrate, 10–15 % protein, and 20–25 % fat), which was identical for each trial. Pre-exercise tests were then completed, followed by the plyometric exercise bout 2 hours after consuming the NSAID or placebo. Four and 24 hours after the completion of the plyometric exercise bout, participants were once again tested for maximum leg strength and vertical jump ability, as well as assessed for muscle soreness in four body regions: shoulder, quadriceps, gluteus maximus, and calves. The rating was measured on a 1-10 visual analogue scale, with zero representing no soreness and ten representing maximal soreness.
What they found
The main findings were as follows:
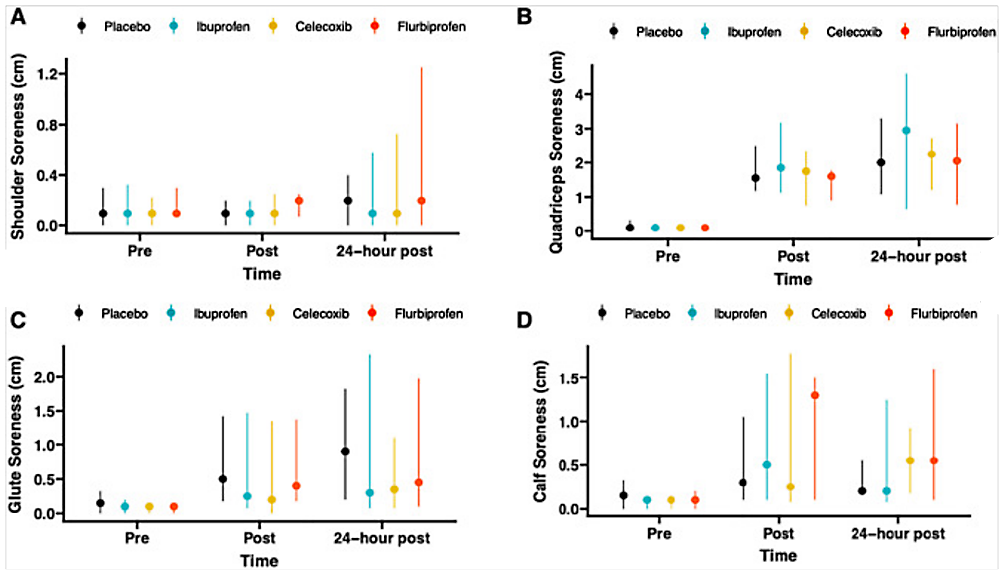
· While the plyometrics exercise increased muscle soreness at 4- and 24-hours post-exercise, there were no significant differences whatsoever between the trials, regardless of whether any of the NSAIDs were taken or the placebo was taken (see figure 1). In other words, taking pre-exercise NSAIDs produced no DOMS benefits at all!
· While vertical jump heights declined in all four trials, there were no differences between trials (in other words, NSAID use conferred no performance benefits).
· Maximum leg strength improved slightly at 4-hours post exercise in the Celecoxib trial, but this benefit disappeared at the 24-hour post-exercise point.
Figure 1: DOMS scores and NSAID/placebo use
Conclusions for athletes
While surprising, the results above are supported by quite early data from elsewhere. For example, Donnelly et al found that a 1200mg dose of ibuprofen taken 30 minutes prior to downhill running had no effect on post-exercise muscle soreness(25). Likewise, another study, by Krentz et al found that 400mg of Ibuprofen ingested after repeated resistance training sessions did not affect ratings of muscle soreness(26). The US Military researchers concluded overall that “NSAIDs did not attenuate post-exercise muscle soreness, or deficits in vertical jump, suggesting NSAIDs such as Ibuprofen and Flurbiprofen may not provide a benefit to reducing muscle soreness or improving post-exercise performance.”
This study is significant because it used a precise methodology and carefully calibrated loading of the muscles during the intense exercise in each of the four conditions. In other words, it compared apples to apples – not to pears! As such, it provides high-quality evidence that NSAID use for reducing DOMS does not yield benefits for athletes, either in terms of soreness or improved jump performance the next day. Returning to the risk-benefits equation, this suggests that athletes who self-medicate with NSAIDs are exposing themselves to proven and significant risks, with little evidence of any benefits. In fact, the supposed benefits could actually be harms, because damping down post-exercise inflammation can interfere with the training adaptation effect!
The only logical advice for athletes at this point in time therefore is that taking NSAIDs to reduce DOMS and speed recovery is not beneficial, potentially harmful and therefore is not recommended. This is particularly the case given that there are safer, more natural and healthier anti-inflammatory options out there for athletes, which have a good body of scientific evidence for their effectiveness. These natural products include curcumin (from turmeric), tart cherry extracts, ginger and omega-3 oils. For a detailed discussion of a more natural approach including supplemental guidelines, readers are strongly advised to see this article. Although aimed at older athletes, this should be considered essential reading for anyone seeking to minimize exercise-associated aches and pains and recover fast!
References
1. J Sports Med Phys Fitness. 2008 Jun;48(2):272-7
2. J Strength Cond Res. 2003; 17: 197-208
3. Scand J Med Sci Sports. 2018; 28: 2252-2262
4. BMC Musculoskelet Disord. 2020; 21: 561
5. J Strength Cond Res. 2014; 28: 74-81.4
6. Mil Med. 2017; 182: e1709-e1712
7. Sports (Basel). 2017 Jan 29;5(1). pii: E11.
8. Front Physiol. 2018 Sep 10;9:1272
9. Clin J Sport Med. 2018 Sep;28(5):427-434
10. Scand J Med Sci Sports 2012. 22: e8-14
11. Spine 1998. 23(7): 834-838 18
12. BMC Musculoskeletal Disorders (2016) 17:383
13. Emerg Med J. 2017 Oct;34(10):637-642
14. J Rheumatology 1999. 26 Supp 56: 18-24, 1999
15. Pain 2000. 85: 169-182 5
16. Aliment Pharmacol Ther 1997. 11: 283-91
17. Scand J Med Sci Sports. 2018 Nov;28(11):2252-2262
18. J Sports Sci. 1999; 17: 197-203
19. J Sports Sci. 1999; 17: 197-203
20. Int. J. Environ. Res. Public Health 2020, 17(14), 5157
21. Med Sci Sports Exerc. 1993; 25: 9-17
22. Am J Sports Med. 2018; 46: 224-233
23. Sports Med Open. 2020; 6: 20
24. J Sci Med Sport. 2024 Feb 13:S1440-2440(24)00050-1. doi: 10.1016/j.jsams.2024.02.002. Online ahead of print
25. Br J Sports Med. 1990; 24: 191-195
26. Appl Physiol Nutr Metab. 2008; 33: 470-475
Newsletter Sign Up
Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Keep up with latest sports science research and apply it to maximize performance
Today you have the chance to join a group of athletes, and sports coaches/trainers who all have something special in common...
They use the latest research to improve performance for themselves and their clients - both athletes and sports teams - with help from global specialists in the fields of sports science, sports medicine and sports psychology.
They do this by reading Sports Performance Bulletin, an easy-to-digest but serious-minded journal dedicated to high performance sports. SPB offers a wealth of information and insight into the latest research, in an easily-accessible and understood format, along with a wealth of practical recommendations.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Performance Bulletin helps dedicated endurance athletes improve their performance. Sense-checking the latest sports science research, and sourcing evidence and case studies to support findings, Sports Performance Bulletin turns proven insights into easily digestible practical advice. Supporting athletes, coaches and professionals who wish to ensure their guidance and programmes are kept right up to date and based on credible science.