You are viewing 1 of your 1 free articles. For unlimited access take a risk-free trial
Breaking point: when running stress gets too much
Trevor Langford looks how runners can identify the early signs of stress fracture, manage an injury once it has occurred and most importantly, reduce the risk of stress fracture to avoid injury in the first place...
Stress fractures are a commonly diagnosed injury in physiotherapy clinics, with studies suggesting that stress fracture accounts for 16% of all running related injuriesSaudi J Sports Med, 2017, 17, 1 - 6. Research has also ascertained that 80-90% of stress fractures occur in the lower limbsOpen Access J Sports Med, 2015, 6, 87 – 95 and that stress fractures are becoming more common with increased exercise participation, and occurring at an earlier age tooSports Health, Nov, 2014, 6, 6, 481 – 491. The purpose of this article is to help you identify the early signs and symptoms of a stress fracture and effectively manage this type of injury. This shouldn’t replace the diagnosis of a physiotherapist or a doctor of course; rather it is designed to help guide you in the right direction.Signs and symptoms
A stress fracture can occur when bone cell depletion outpaces the laying down of new bone cells, which results in a weakened bone structureEpidemiol Rev, 2002, 24, 2, 228 - 247. This can happen when someone begins a new activity, but can also arise in experienced athletes too, when the load is dramatically increased.It is essential to be aware of what to look for if you suspect stress fracture. A stress fracture of the lower leg typically presents with swelling, redness, heat and pain, which is aggravated by running or loading, and which eases with rest or reduced load. Tenderness at the bone site is present on palpation (pressing).
A ‘hop test’ is often included in a clinical assessment to determine the intensity of pain and how much load if any the patient is able to withstandAm Fam Physician, 2011, Jan, 83, 1, 39 - 46. In this test, you stand on one foot (of the leg that hurts) and hop. As a very rough (but unscientific) guide, if you can hop on it, it is probably not a stress fracture (if it is a stress fracture, the pain will not be tolerable). However, a hop test would not be carried out on someone who had severe pain on walking and ascending/descending stairs.
Common causes
Box one highlights a variety of the factors that are known to be associated with stress fracture. Athletes, and sometimes coaches alike, often take the approach to ‘push through pain’ – either because curtailing training may be perceived as a sign of weakness or because they are unaware of the implications surrounding it. Muscle fatigue is to be expected following a heavy training session, and this should be managed using recovery strategies. However, pain affecting a bone should be very carefully monitored. Ignoring the onset of a niggle (perhaps because a big event is on the horizon), can be a common reason why a stress fracture is sustained. If a niggle does present, it’s essential to manage it appropriately using ice and soft tissue release around the involved bone - but most importantly by modification of bone loading.Barefoot running
Barefoot running or using minimalist footwear (see figure 1) is a big topic of discussion among the running community, and one that often raises questions about stress fracture risk. In terms of the stress fracture incidence, it is an important factor to consider when weighing up the benefits. A relatively recent study used a questionnaire to ask 509 runners with experience of barefoot running their feedbackJ of sport and health sci, 2014, 3, 131 – 136. The results showed that 55% of the respondents had Achilles tendon or forefoot pain initially, and of these participants, 47% reported that their pain subsided relatively quickly. It was also reported that the incidence of stress fractures to the metatarsal bones of the foot as a result of barefoot or minimalist footwear is comparatively rare. However, other recent research suggests that higher volumes (20+kms per week) of minimalist shoe training – particularly in heavier runners (85kg plus) – can increase the risk of injuryAm J Sports Med. 2017 Jan 1:363546516682497. doi: 10.1177/0363546516682497.BOX 1: RISK FACTORS ASSOCIATED WITH THE OCCURRENCE OF A STRESS FRACTURESaudi J Sports Med, 2017, 17, 1 - 6 Open Access J Sports Med, 2015, 6, 87 – 95 Sports Health, Nov, 2014, 6, 6, 481 – 491
Intrinsic factors
- Females - Irregular menstrual cycle in females and use of a contraceptive pill.
- Age – Older athletes being at greater risk.
- Race – White athletes are more at risk than black athletes.
- Anatomy – high foot arches increase risk compared to lower foot arches.
- Gait – Poor running gait increases stress fracture risk.
- Bone – Reduced bone mineral density (BMD) and reduced bone width.
- Aerobic fitness – slower runners at greater risk of stress fractures due to increased foot contact.
- Nutrition – deficits in certain nutrients can predispose to stress fractures.
- Sedentary lifestyle – those living an inactive lifestyle prior to starting running.
- Smoking
- Previous injuries – Those suffering previous stress fractures are at greater risk of subsequent fracture.
Extrinsic factors
- Type of sport – Runners are particularly susceptible to stress fractures.
- Physical load – Those who cover higher mileage are more likely to be diagnosed with a stress fracture.
- Footwear – Age/mileage of training shoes (older/high-mileage shoes increase risk).
- Training / playing surface – Hard surfaces increase risk.
FIGURE 1: EXAMPLE OF MINIMALIST FOOTWEAR

Vibram ‘Five Fingers’ minimalist shoes
Commonly affected locations
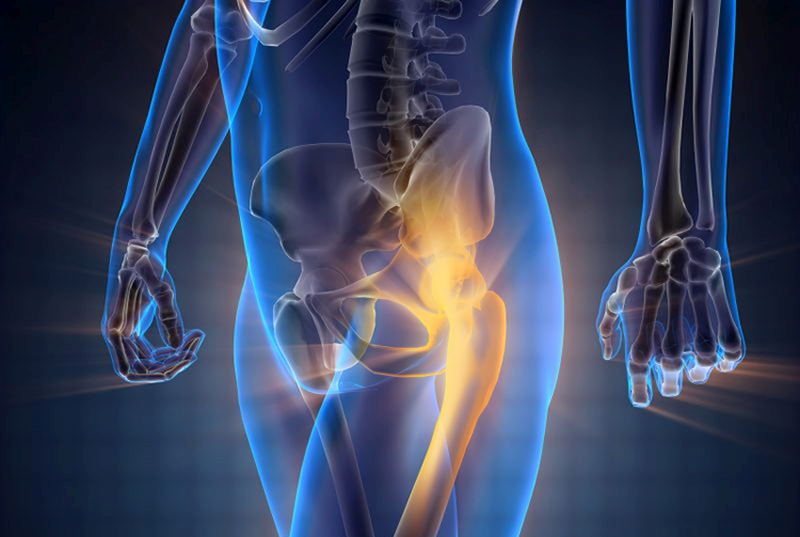
A stress fracture can occur in any one of a number of locations throughout the body and excessive repetition of an exercise can predispose to bone failure. However, due to the constant repetition of the foot striking the ground during running, it is easy to understand how stress is directed to the lower limb - more so than in the hips, pelvis or the spine. The tibia of the lower leg has been reported to be the most commonly affected bone with a stress fracture incidence rate of 23.6%, with the fibula bone (also in the lower leg) being up to 23%. The navicular bone in the foot has an incidence of 17.6%, the metatarsal bones in the foot 16.2%,the femur (thigh bone) 6.6%, and the pelvis just 1.6%Saudi J Sports Med, 2017, 17, 1 - 6 Open Access J Sports Med, 2015, 6, 87 – 95 (see figure 2).FIGURE 2: STRESS FRACTURE – RISK BY LOCATION
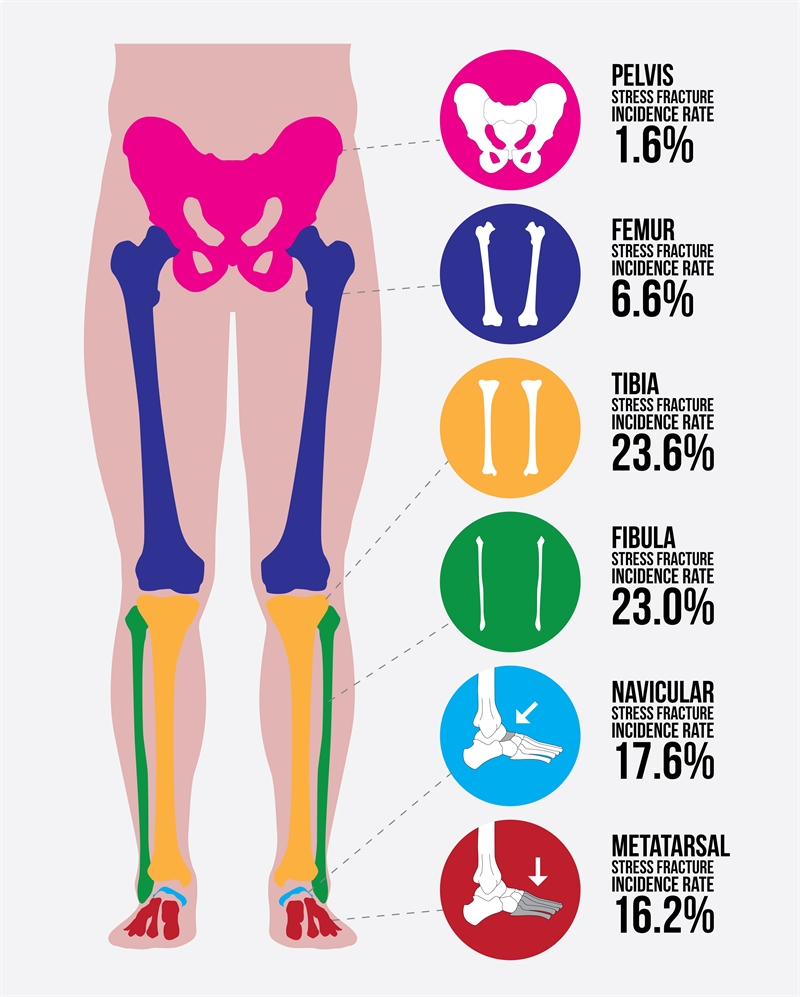
Tibia-related stress fractures are most commonly sustained on the inside of the larger bone in the lower leg, nearest the footSaudi J Sports Med, 2017, 17, 1 - 6. It is less common for a stress fracture to occur in the mid part and at the front of the tibia bone in runners. Recreational runners are more susceptible to sustaining a stress fracture on the inside of the tibia bone nearest to the ankleSaudi J Sports Med, 2017, 17, 1 - 6. Tibial stress fractures affecting the mid shaft of the tibia bone at the front are much less frequent and can be running career threatening injuries. Furthermore, stress fractures at the front of the tibia bone may arise from jumping actions or activities involving a variety of movements such as trail running with uneven groundSaudi J Sports Med, 2017, 17, 1 - 6.
Stress fractures can occur in the spine as well as the legs but these types of injuries tend to occur mainly in sports involving single-sided loading with rotation such as football, cricket, rowing, gymnastics and tennis. As running is an activity that provides equal loading to both limbs, a spinal-related stress lesion is much less likely in runners.
Management and prevention
It is essential to manage a stress fracture correctly, and the very first thing to do is reduce physical loading to the involved area. This can be achieved firstly by stopping the aggravating activity - ie running. It is important for runners to realise that delayed action is likely to lead to a more prolonged injury and a greatly delayed return to runningAm Fam Physician, 2011, Jan, 83, 1, 39 - 46.If you feel pain when walking, then loading should be reduced further by using crutches to relieve some of the weight from the lower limbs. During the acute stage, when swelling, heat, redness and pain are evident, ice should also be used hourly for 15 minutes at a time to reduce the signs of inflammation. During this stage, you can maintain cardiovascular fitness by doing upright water running, stationary biking or upper body biking.
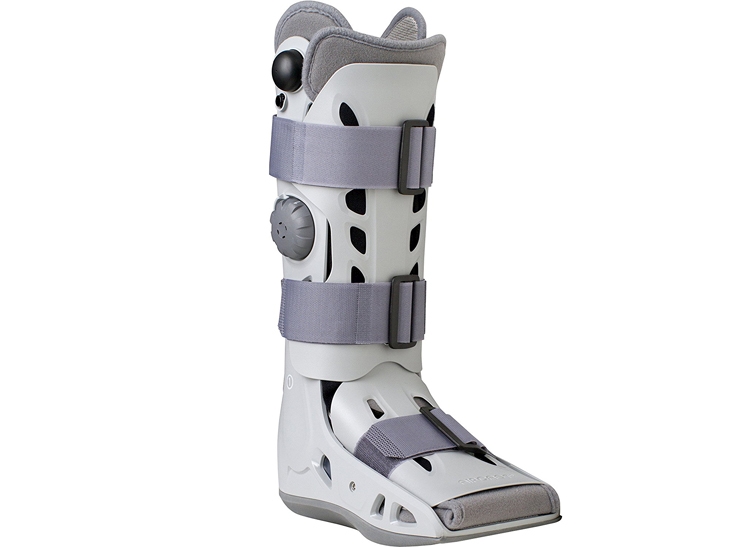
Analgesic such as acetaminophen (Paracetamol) or non-steroidal anti-inflammatories (NSAIDs) may be prescribed for pain management. However, caution is required as there is some evidence that NSAIDs could inhibit fracture healingAm Fam Physician, 2011, Jan, 83, 1, 39 - 46. Fracture healing can take between four and twelve weeks before a return to training is possible. During this time, you will need to be reassessed every two to three weeks in order to monitor pain intensity and level of functioning. As pain reduces, loading can be gradually increased in a controlled manner. There is some suggestion that by using a pneumatic brace or ‘aircast boot’, (figure 3) return to training can be significantly faster, but more evidence is required before we can be sure of thisAm Fam Physician, 2011, Jan, 83, 1, 39 - 46.
FIGURE 3: EXAMPLE OF AIRCAST BOOT
Warning signs
A stress fracture often builds over a period of time, and can often appear as a ‘niggle’ over an area of bone. These minor niggles are often brushed off as nothing, and training is continued while the ‘niggle’ evolves into something more prominent and longer lasting. It is at this point that an athlete (who can be someone starting a ‘couch-potato to 5km fun run’ programme or an Olympic athlete - they are both challenging their body, just at different intensities) should listen to their body.It is a wise approach to keep a log of your running distances, times, dates, and if pain appears, rate it using a pain scale (zero being no pain and 10 being high pain). This can help a physiotherapist identify a trend in a training plan where an overload has taken place. Using an online app for recording this data can also be a really helpful tool for a physiotherapist to study. Sometimes when a stress fracture presents – for example at the hip joint - there may be referred pain into the surrounding structures. It is essential to not assume that pain in one area automatically means that the problem resides in that area.
If a stress fracture is suspected, it is essential to obtain a form of imaging either through an X-ray or MRI scan. An MRI scan will provide much greater detail than an X-ray but X-ray scans may be the preferred option initially, because of their low cost and increased availability. Either way, a scan will help the physiotherapist to formulate a rehabilitation plan based on the clinical presentation and where pain presents in addition to imaging report.
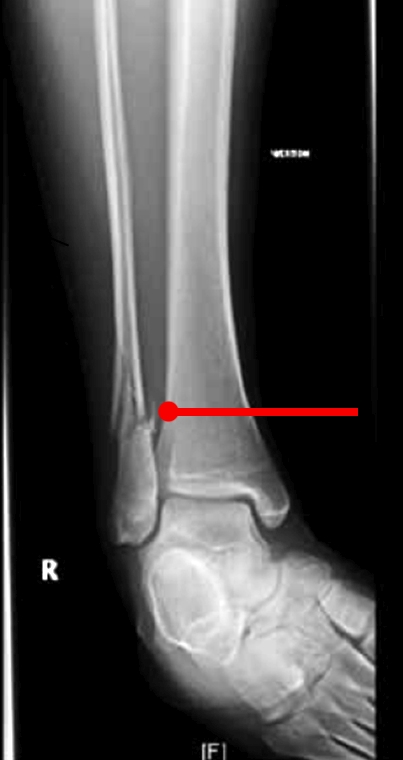
FIGURE 4: FRACTURE OF THE FIBULAR BONE IMMEDIATELY POST-RACE, INDICATED BY RED POINTER
CASE STUDY: Stress fracture in an elite cross-country runner

A relatively recent report documented a stress fracture in an elite cross country runner with nutritional deficitsThe J of the Malta Coll of Fam Doc, Dec, 2015, 4, 3, 6 – 10. An adolescent female runner selected by the Maltese Olympic team (name withheld for confidentiality reasons) was due to race in a 3.5k run six months later. During the six-month period of intense training, she ran up to four hours per week, much of which was interval training.
During the first three months of training, the runner noticed lower leg shin pain on the inside of both her right and left sides. The pain was described as nagging but it didn’t limit her training and she continued to proceed. The symptoms were aggravated by running, and were alleviated by rest. A physiotherapist was consulted who advised adapting her running gait, using strapping and performing calf stretches. However, these had no effect on the pain. The pain was at its most intense just a few days prior to the 3.5k competition and she didn’t want to seek further medical advice for fear of being withdrawn. During this period, she had some persistent swelling on the lower right leg on the inside of the tibia bone.
During the race itself, she recalled feeling a sharp increase in pain in her lower right leg ,similar to the feeling of ‘being kicked in the shin’. She managed to complete the race and had a sprint finish over 500 metres at the end too. On crossing the finish line, the athlete noticed that she had a significant amount of swelling on her lower right leg. A sports doctor suspected a stress fracture based on her symptoms and an X-ray indicated a complete fracture of the lower right fibula (figure 4).
The patient’s lower leg was immobilised in plaster for six in which a review was carried out. After six weeks there was evidence of delayed union of the bone and therefore a further x-ray was taken at nine weeks, which indicated bone healing. Although she was given a medical history form to complete upon selection, her nutritional deficits were not taken into account. While she maintained a balanced nutritional intake, she lacked in dairy and meat products (especially red meat) and took no supplementary products. She was prescribed calcium (important for bone health) and iron tablets and advised to eat foods rich in calcium and iron nutrients. She was also measured for some orthotic insoles to help reduce further stress to the foot. She eventually went on to make a full recovery.
Newsletter Sign Up
Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Keep up with latest sports science research and apply it to maximize performance
Today you have the chance to join a group of athletes, and sports coaches/trainers who all have something special in common...
They use the latest research to improve performance for themselves and their clients - both athletes and sports teams - with help from global specialists in the fields of sports science, sports medicine and sports psychology.
They do this by reading Sports Performance Bulletin, an easy-to-digest but serious-minded journal dedicated to high performance sports. SPB offers a wealth of information and insight into the latest research, in an easily-accessible and understood format, along with a wealth of practical recommendations.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Performance Bulletin helps dedicated endurance athletes improve their performance. Sense-checking the latest sports science research, and sourcing evidence and case studies to support findings, Sports Performance Bulletin turns proven insights into easily digestible practical advice. Supporting athletes, coaches and professionals who wish to ensure their guidance and programmes are kept right up to date and based on credible science.